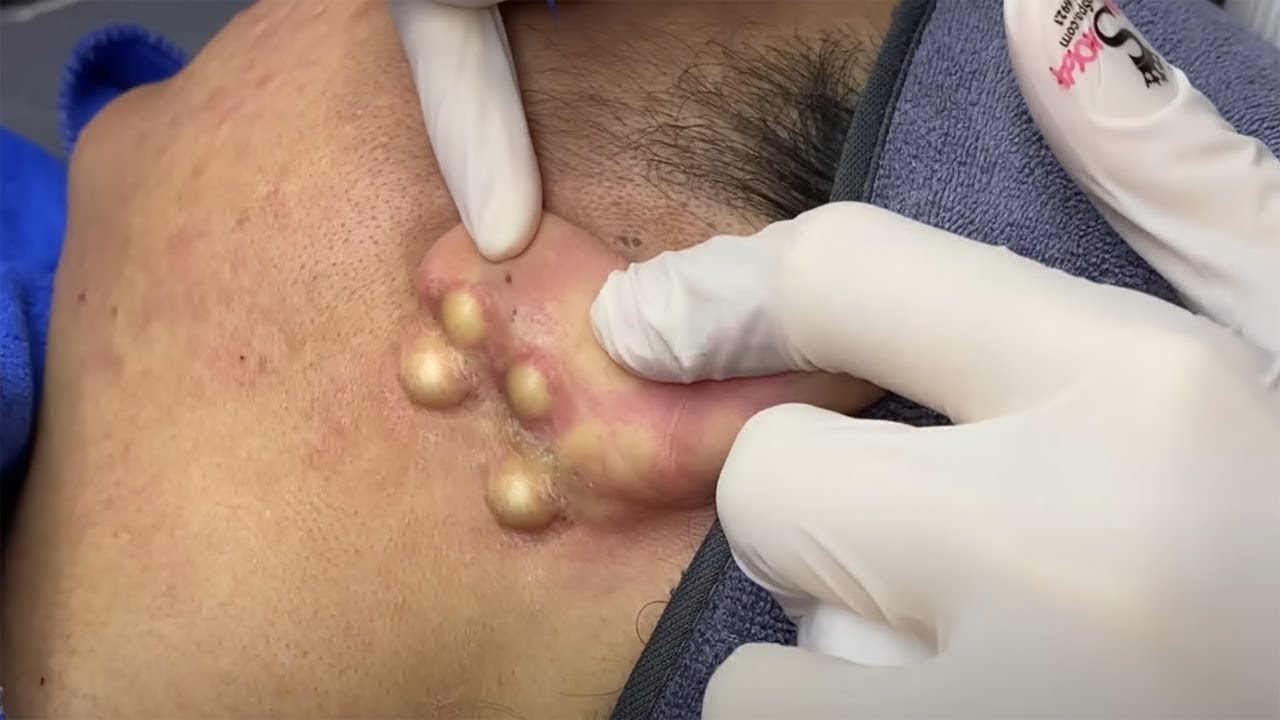
Blackhead Removal without Extractor Tool (Edited) | Auburn Medical Group
Blackhead Removal: The Most Satisfying Extraction Ever!
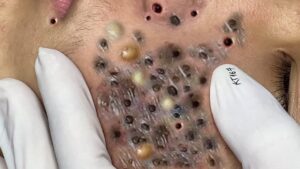
Hormonal acne is a challenging and often emotionally draining condition that affects an estimated three in ten adults. It can undermine confidence, disrupt daily life, and persist for years without proper intervention. Despite its frustrating nature, hormonal acne is treatable with science-backed solutions guided by dermatology professionals. Understanding what hormonal acne is, why it happens, and which treatments are effective is the first step toward long-term, manageable results.
Hormonal acne, also called adult female acne, is a form of acne vulgaris that primarily affects women over 25. It differs from teenage acne in both its causes and patterns. While teen acne is often centered on the T-zone, hormonal acne typically appears along the jawline, chin, and lower cheeks in a distinctive “U-shaped” pattern. These breakouts often consist of painful, inflamed nodules or cysts that do not come to a head. Symptoms may persist year-round but tend to worsen cyclically around menstruation due to hormonal fluctuations.
This form of acne is driven by elevated androgen levels (hyperandrogenism). Androgens, such as testosterone, are necessary for healthy female reproductive function, but excessive levels stimulate the skin’s sebaceous glands to overproduce oil, leading to clogged pores and deep cystic lesions. Hormonal acne can arise during a range of life stages, including pregnancy, postpartum, changes in contraceptives, or perimenopause. Conditions such as PCOS and hirsutism also increase susceptibility. Stress is another significant contributor; prolonged elevated cortisol levels can heighten androgen activity and exacerbate breakouts. Diet may play a role as well, particularly high-glycaemic foods that spike blood sugar and trigger inflammation.
Unlike surface-level teen acne, hormonal acne is internal in origin, which is why DIY treatments and over-the-counter products rarely provide lasting relief. Untreated hormonal acne can leave long-term marks such as post-inflammatory hyperpigmentation or scarring, making early professional intervention essential.
Treatment plans vary depending on severity. For mild to moderate cases, dermatology professionals typically recommend topical treatments such as benzoyl peroxide, retinoids (like adapalene or tretinoin), and azelaic acid. Benzoyl peroxide reduces bacteria and inflammation but must be used carefully due to its fabric-bleaching effect. Retinoids improve cell turnover, unclog pores, and reduce pigmentation, though they require consistent use and are unsuitable during pregnancy or breastfeeding. Azelaic acid is a gentler option ideal for sensitive skin or those who cannot use stronger prescriptions.
For severe or persistent hormonal acne, oral treatments may be necessary. Dermatologists often prescribe oral antibiotics to quickly reduce inflammation and bacterial activity, typically for a limited period to prevent resistance. These are combined with topical treatments for comprehensive management and faster clearing of cystic lesions. The goal is to gain rapid control of active breakouts, reduce the risk of scarring, and then maintain clear skin with long-term topical therapy.
Ultimately, hormonal acne is a medical condition that requires targeted, personalised care. With the correct combination of topical and oral treatments, simplified skincare routines, and professional guidance, long-term improvement is achievable.
If you’d like, I can also convert this into a shorter 300-word summary, create an SEO-focused version, or format it for a blog article.